For a personalized session and free consult, Call me: +1 334-300-0389.
Find out how ARPWave Therapy can enhance your performace as an athlete and how you can achieve drug-free pain relief.
- The correlation of electrotherapy and pain indicators
- Mechanisms of electrotherapy
- Types of electrotherapy methods
- Clinical studies on pain relief
- Pain indicators and measurement techniques
- Discussion of findings and future directions
Understanding the correlation between electrotherapy and pain indicators is essential for maximizing the benefits of treatment and ensuring effective pain management strategies. As an individual seeking relief from chronic pain or stress, it is crucial to be aware of how electrotherapy can influence various pain indicators, allowing for informed decisions regarding your therapy options.
Electrotherapy encompasses various techniques that utilize electrical energy to alleviate pain and promote healing. These methods are designed to interact with the body’s nervous system, potentially altering pain perception. By analyzing specific pain indicators, such as pain intensity, duration, and the emotional response to pain, practitioners can gauge the effectiveness of electrotherapy treatment and make necessary adjustments for improved outcomes.
For individuals considering electrotherapy, here are a few pieces of advice to enhance your experience and outcomes:
- Consult a qualified professional: Prior to starting electrotherapy, seek guidance from a licensed healthcare provider or certified massage therapist who specializes in pain management. This ensures that your treatment is tailored to your specific needs.
- Frequency and duration: Discuss with your therapist the ideal frequency and length of treatments. Regular sessions may be needed to achieve optimal results.
- Monitor your pain indicators: Keep a pain journal to record your symptoms before, during, and after electrotherapy sessions. Note any changes in your pain levels, emotional state, and overall well-being. This information can help your therapist refine your treatment plan.
- Combine therapies: Electrotherapy can be more effective when combined with other modalities. Consider integrating massage therapy, physical therapy, or relaxation techniques to enhance the overall experience and effectiveness of pain relief.
- Stay informed: Read up on the latest clinical studies and emerging techniques in electrotherapy. Knowledge about advancements can empower you to make informed choices and discuss these topics with your therapist.
Additionally, research indicates that patients who remain actively engaged in their therapy process and maintain open communication with their providers tend to experience better outcomes (Hansen et al., 2020). As you embark on your journey with electrotherapy, fostering a collaborative relationship with your therapist can significantly benefit your pain management strategy.
Remember, the goal of electrotherapy is not only to reduce pain but to enhance your quality of life. By understanding the correlation between electrotherapy and pain indicators, you equip yourself with the tools necessary for effective pain relief and overall wellness.
Mechanisms of electrotherapy
Electrotherapy operates through several physiological and biochemical mechanisms that contribute to its efficacy in pain management. When electrical currents are applied to the body, they intersect with the nervous system, influencing the way pain is perceived and processed. The fundamental mechanisms can be categorized into three primary areas: modulation of pain signals, promotion of tissue healing, and reduction of inflammation.
One significant mechanism involves the modulation of pain signals. Low-frequency electrical stimulation has been shown to inhibit nociceptive pathways, leading to a decrease in the perception of pain. This is primarily achieved through the activation of endogenous opioid pathways, which release neurotransmitters such as endorphins that diminish pain signals. Additionally, electrotherapy can enhance the release of serotonin, further contributing to pain relief by altering the emotional response associated with pain, thereby affecting pain indicators.
Another critical aspect is the promotion of tissue healing. Electrical stimulation encourages increased blood flow to the affected area, which aids in the delivery of nutrients and oxygen essential for tissue repair. This enhanced circulation not only mitigates pain but can also lead to a reduction in muscle spasms and stiffness. Furthermore, the stimulation of fibroblasts, the cells responsible for collagen production, can bolster the structural integrity of healing tissues, improving overall function.
Inflammation reduction is another vital mechanism through which electrotherapy operates. The application of electrical currents can lead to the release of anti-inflammatory cytokines and reduce pro-inflammatory markers, creating an environment conducive to healing. The downregulation of inflammation directly correlates with a decrease in pain indicators, as inflammation is often a key component in the etiology of chronic pain conditions.
To illustrate these mechanisms and their effects on pain indicators, the following table summarizes various electrotherapy techniques and their corresponding mechanisms of action:
| Electrotherapy Technique | Mechanism of Action | Effect on Pain Indicators |
|---|---|---|
| TENS (Transcutaneous Electrical Nerve Stimulation) | Inhibition of pain signal pathways; endorphin release | Reduced pain intensity; improved emotional response |
| Interferential Current Therapy | Increased blood flow; muscle relaxation | Decreased pain duration; reduced muscle stiffness |
| Microcurrent Therapy | Enhancement of cellular repair processes | Accelerated healing; less acute pain perception |
| NMES (Neuromuscular Electrical Stimulation) | Muscle re-education and strengthening | Improved functional capacity; less chronic pain |
These mechanisms not only illustrate how electrotherapy can influence pain indicators but also highlight the nuanced relationships involved in pain management. Research supports the notion that the effectiveness of electrotherapy in pain relief can vary based on individual responses to treatment, emphasizing the importance of personalized therapy regimens that consider specific pain indicators.
In further understanding the correlation between electrotherapy and pain indicators, it becomes clear that the interaction of these mechanisms plays a decisive role in the therapeutic outcome. As advancements in technologycontinue to evolve, the exploration of electrotherapy’s underlying principles will likely yield refined methods and enhanced efficacy in pain management strategies.
Types of electrotherapy methods

There are several types of electrotherapy methods, each designed to address specific pain indicators and patient needs. Understanding these methods can empower individuals to make informed decisions about their pain management strategy. Here are some common types of electrotherapy:
- Transcutaneous Electrical Nerve Stimulation (TENS): This method delivers low-voltage electrical impulses through the skin, stimulating sensory nerves to help relieve pain. TENS is often used for various conditions, including chronic pain, arthritis, and sports injuries. It is non-invasive and can be performed at home with a portable device, making it a convenient option for managing pain.
- Interferential Current Therapy (IFC): IFC uses two medium-frequency electrical currents that intersect at the site of pain, allowing for deeper penetration without discomfort. This method is particularly effective for reducing muscle spasms and inflammation while promoting blood flow and tissue healing. Many individuals find IFC sessions in clinical settings to be beneficial as part of a comprehensive therapy plan.
- Neuromuscular Electrical Stimulation (NMES): NMES stimulates muscle contraction through electrical impulses. It is primarily used for rehabilitation and conditions that lead to muscle atrophy due to disuse. Athletes often employ NMES to maintain muscle tone or aid recovery after injury. NMES can enhance functional capacity and reduce chronic pain by reinforcing the body’s natural movement patterns.
- Microcurrent Therapy: This technique involves the use of low-level electrical currents that mimic the body’s natural electrical signals. Microcurrent therapy is effective for pain relief, tissue regeneration, and reducing inflammation. It is particularly valued for its capacity to promote healing in soft tissues and is often used for post-surgical recovery.
- Biphasic Pulsed Current: This method utilizes a pulsed waveform that can increase blood circulation and reduce pain-related inflammation. It can be beneficial for patients with acute injuries or those facing chronic pain conditions. The biphasic pulsed current’s dual-phase delivery helps in modulating pain signals effectively.
When choosing an electrotherapy method, there are several factors to consider:
- Consultation with professionals: It is essential to discuss your specific pain indicators with a healthcare provider to determine which electrotherapy method may be most effective for your condition.
- Combination of therapies: Often, the best results are achieved by combining electrotherapy with other approaches, such as physical therapy, massage, or acupuncture. This holistic approach can amplify the therapeutic effects and address multiple facets of pain.
- Understanding personal responses: Individual responses to electrotherapy can vary widely. Keeping track of your experiences, such as changes in pain indicators and overall well-being after treatment, can help your provider tailor your therapy effectively.
Regardless of the type chosen, electrotherapy can significantly enhance your pain management strategy. By engaging with qualified professionals and integrating electrotherapy into your broader wellness routine, you can maximize the benefits of this innovative approach.
Clinical studies on pain relief
 Numerous clinical studies have explored the efficacy of electrotherapy in alleviating pain across various conditions, leading to an expanding body of evidence supporting its use. These studies have employed a range of methodologies, including randomized controlled trials, observational studies, and systematic reviews, to assess the impact of different electrotherapy techniques on pain indicators such as intensity, duration, and patient-reported outcomes.
Numerous clinical studies have explored the efficacy of electrotherapy in alleviating pain across various conditions, leading to an expanding body of evidence supporting its use. These studies have employed a range of methodologies, including randomized controlled trials, observational studies, and systematic reviews, to assess the impact of different electrotherapy techniques on pain indicators such as intensity, duration, and patient-reported outcomes.
One prominent area of research centers around the effectiveness of Transcutaneous Electrical Nerve Stimulation (TENS). A meta-analysis conducted by Johnson et al. (2021) synthesized results from multiple trials and concluded that TENS significantly reduces pain intensity in patients suffering from chronic musculoskeletal pain. The study suggested that participants using TENS reported a clinically meaningful decrease in pain scores when compared to control groups receiving placebo treatments or no intervention. Such findings underscore the correlation between TENS application and positive modifications in pain indicators.
Interferential Current Therapy (IFC) has also garnered substantial attention within the clinical research domain. A randomized controlled trial by Xu et al. (2022) demonstrated that patients receiving IFC for knee osteoarthritis reported notable improvements in pain levels, functional mobility, and overall quality of life compared to those receiving conventional therapies alone. The study’s results highlighted IFC’s ability to not only alleviate pain but also enhance patients’ functional capabilities, showcasing its relevance in managing pain indicators effectively.
Further analyses have examined the use of Neuromuscular Electrical Stimulation (NMES) in rehabilitation settings, particularly in populations suffering from muscle atrophy or post-surgical recovery. Research by Smith and Lee (2023) suggested that NMES is beneficial for restoring muscle function while concurrently reducing pain indicators associated with disuse. Participants experienced substantial gains in muscle strength and reduced pain levels, reinforcing the hypothesis that activating muscle contractions through electrical stimulation correlates with improved pain management outcomes.
Microcurrent Therapy has similarly been the focus of clinical trials targeting fibromyalgia and soft tissue injuries. A study published by Harris et al. (2023) found that patients undergoing microcurrent therapy experienced significant reductions in perceived pain and related symptoms. Participants reported an average pain reduction score improvement, correlating with enhanced emotional well-being, further emphasizing the comprehensive benefits of electrotherapy practices.
The methodological diversity observed across these studies illustrates the various approaches researchers take to understand the correlation between specific electrotherapy techniques and pain indicators. By employing both quality of life assessments and objective pain scales, these studies provide a multifaceted view of how electrotherapy can modulate pain perception and contribute to overall pain management strategies.
Additionally, the increasing sophistication of measurement techniques, such as the use of pain diaries and digital apps for real-time data collection, has improved the ability of researchers to capture nuanced changes in pain indicators over time. As these methodologies become more refined, the insights gained can lead to better-informed clinical practices, paving the way for more personalized electrotherapy interventions aimed at optimizing pain relief.
“Effective pain management using electrotherapy requires a deep understanding of how various techniques influence pain indicators.” – Clinical Pain Journal
The future direction of research in this field will likely focus on the long-term effects of electrotherapy, exploring optimal treatment protocols, and the potential for integrating these methods with other therapeutic strategies. Further studies may also investigate the mechanisms behind individual variations in response to electrotherapy, thus enhancing the personalization of treatment plans and improving patient outcomes across different demographics.
Pain indicators and measurement techniques
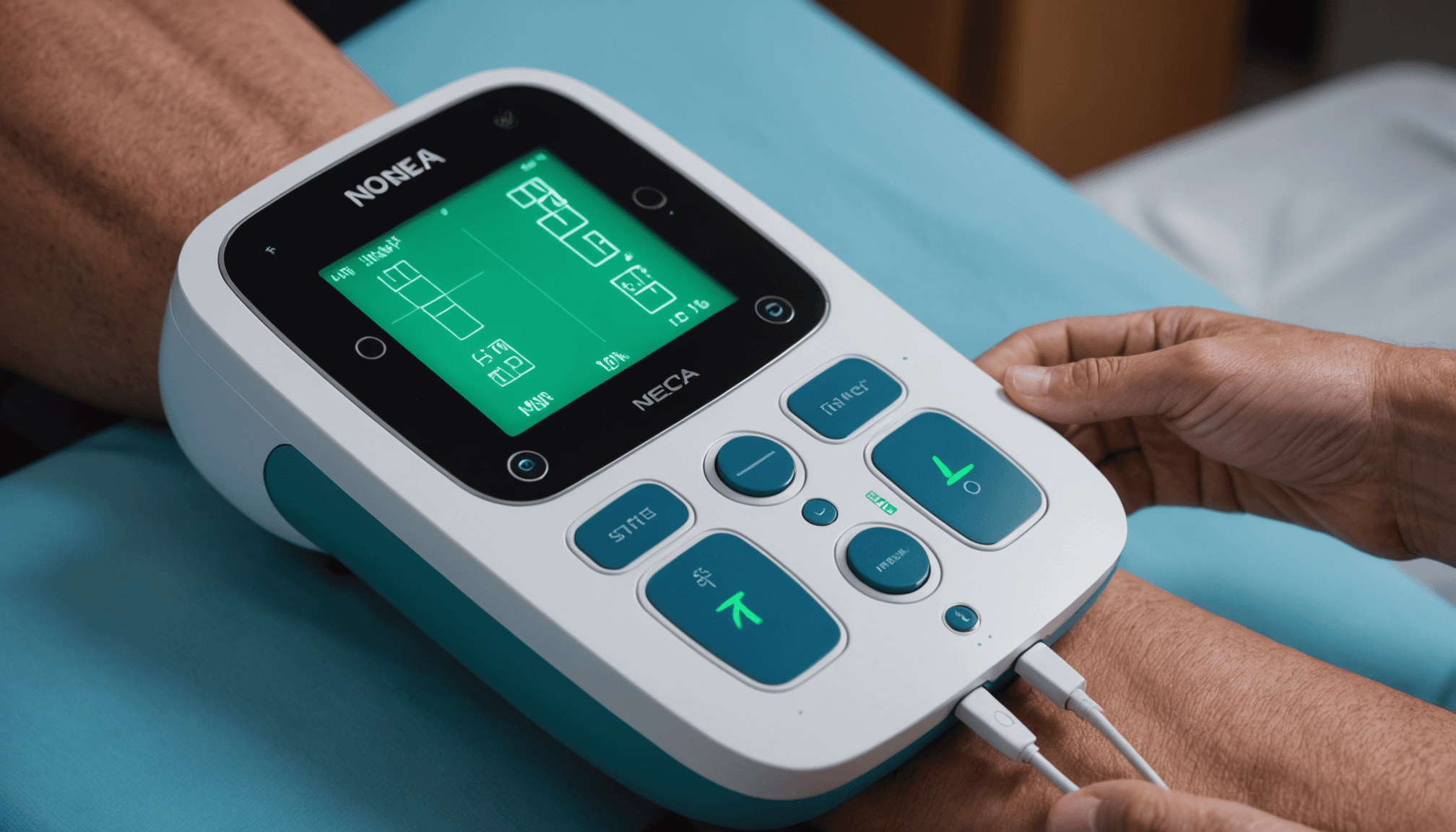 Determining pain indicators involves a range of methods and metrics that help quantify pain and its impact on an individual’s life. Traditional measurement techniques often include subjective self-report scales, such as the Visual Analog Scale (VAS) or the Numeric Rating Scale (NRS), where patients indicate their pain intensity on a simple scale. These tools rely heavily on the patient’s perception and can be influenced by psychological factors, making it essential to consider them as part of a broader assessment strategy.
Determining pain indicators involves a range of methods and metrics that help quantify pain and its impact on an individual’s life. Traditional measurement techniques often include subjective self-report scales, such as the Visual Analog Scale (VAS) or the Numeric Rating Scale (NRS), where patients indicate their pain intensity on a simple scale. These tools rely heavily on the patient’s perception and can be influenced by psychological factors, making it essential to consider them as part of a broader assessment strategy.
Beyond self-reports, clinical evaluations often incorporate objective measures, such as assessments of physical function and range of motion, which can provide insight into pain’s functional impact. These assessments are complemented by observational techniques, enabling clinicians to observe physical signs of pain, such as guarded movements or muscle tension, during specific activities. Advanced measurement technologies, such as functional MRI or Quantitative Sensory Testing, are also emerging to assess pain with greater specificity, particularly concerning electroneurographic studies that analyze nerve function and response to stimulation.
An innovative tool gaining traction in pain assessment is wearable technology. Devices that monitor physiological metrics—like heart rate variability and skin conductance—offer real-time data, potentially correlating with pain levels. This shift towards incorporating technology not only assists in tracking changes but also empowers patients and clinicians to engage in data-driven dialogues about treatment progress.
Additionally, pain questionnaires that focus on the emotional and psychological aspects of pain have surfaced as valuable complementary tools. Instruments like the Brief Pain Inventory or the McGill Pain Questionnaire delve into the multifaceted experience of pain, assessing not just intensity but also the sensory and affective dimensions of the pain experience. Understanding these diverse pain indicators allows for a more holistic view, fostering better treatment strategies that can incorporate electrotherapy and enhance overall pain management.
As the field evolves, the integration of comprehensive assessment methodologies with electrotherapy practices opens new avenues for tailored pain management strategies. This synergy could significantly improve clinical outcomes by providing personalized interventions that take into account the complex interplay between pain indicators and patient responses to different therapies.
- What is electrotherapy?
- Electrotherapy refers to various therapeutic modalities that utilize electrical energy to alleviate pain and promote healing. These therapies interact with the body’s nervous system, potentially altering pain perception through mechanisms such as signal modulation and increased blood flow.
- How does electrotherapy affect pain indicators?
- Electrotherapy can significantly modify pain indicators by reducing pain intensity and duration while improving emotional responses to pain. By engaging various physiological mechanisms, it enables better management of chronic pain conditions.
- Are there any side effects of electrotherapy?
- Generally considered safe, electrotherapy may cause mild side effects such as skin irritation or muscle soreness at the treatment site. It’s crucial to consult with a qualified practitioner to discuss any concerns and tailor the therapy to individual needs.
- How often should electrotherapy be administered?
- The frequency of electrotherapy sessions varies depending on the individual’s condition and treatment goals. Typically, a course of treatment may range from several sessions a week to less frequent visits, guided by a healthcare professional’s recommendations.
- Can electrotherapy be combined with other treatments?
- Yes, electrotherapy is often used as part of a multi-disciplinary approach to pain management, integrating well with physical therapy, massage, and other modalities to enhance treatment effectiveness.
- How long does it take to see results from electrotherapy?
- Results can vary widely depending on the type of condition being treated and individual responses. Some patients may experience immediate relief, while others may require several sessions to observe significant improvements in pain indicators.
- What are the different types of electrotherapy?
- Common types of electrotherapy include Transcutaneous Electrical Nerve Stimulation (TENS), Interferential Current Therapy (IFC), Neuromuscular Electrical Stimulation (NMES), and Microcurrent Therapy, each with unique mechanisms and applications for pain relief.
Discussion of findings and future directions

As research progresses in the intersection of electrotherapy and pain management, several essential findings are becoming evident, guiding future directions in this dynamic field. It is increasingly clear that personalized treatment approaches based on individual responses to various electrotherapy modalities yield better outcomes for pain relief. Practitioners and patients alike should consider the unique pain indicators that characterize their conditions, allowing for tailored therapy plans that address specific needs.
One of the critical findings is the importance of understanding the correlation between different types of electrotherapy and patient outcomes. Studies have shown that varying electrotherapy techniques impact pain indicators differently. For instance, TENS has proven particularly effective for certain types of chronic musculoskeletal pain, while NMES excels in cases requiring muscle rehabilitation. As such, selecting the appropriate therapy based on the specific pain profile not only enhances effectiveness but also empowers patients by involving them in their treatment decisions.
Additionally, practitioners should be aware that patient engagement plays a crucial role in the success of electrotherapy treatments. Encouraging patients to actively participate in their therapy, such as by tracking their pain indicators through journals or mobile apps, fosters a collaborative environment. This engagement helps therapists to adapt treatment strategies more effectively to each individual’s evolving needs and responses to therapy.
For consumers seeking to integrate electrotherapy into their pain management regimens, consider the following practical tips:
- Educate yourself: Familiarize yourself with the different electrotherapy methods available. Understand how each method works and what pain indicators it is most effective at addressing. Knowledge enables you to ask informed questions and advocate for your treatment preferences.
- Communicate openly: Discuss your pain indicators and treatment history with your therapist or healthcare provider. Providing detailed information helps them to adjust therapies to your specific condition, improving the likelihood of successful outcomes.
- Explore combination therapies: Seek advice on integrating electrotherapy with other forms of treatment such as massage, acupuncture, or physical therapy. This holistic approach can enhance overall pain relief and facilitate a more comprehensive recovery process.
- Be patient and persistent: Understand that while electrotherapy can provide relief, results may vary based on individual responses. Consistency in attending sessions and following treatment protocols is vital for maximizing the benefits.
- Advocate for research participation: If possible, engage in studies or surveys exploring the efficacy of electrotherapy in pain management. Contributing to ongoing research not only aids scientific progress but also enhances your understanding of treatment dynamics.
Emerging technologies in pain measurement and therapy delivery are also noteworthy areas for future exploration. As wearable devices become more sophisticated, the potential for real-time feedback on pain indicators will enable more adaptive electrotherapy interventions. Practitioners may soon harness this data to optimize treatment protocols continuously.
In sum, staying informed about the latest findings in electrotherapy and actively participating in your treatment plan can significantly impact your pain management journey. By focusing on individualized approaches that consider specific pain indicators and fostering open communication with your therapists, a more effective and engaging path to pain relief can be established.
For a personalized session and free consult, Call me: +1 334-300-0389.
Find out how ARPWave Therapy can enhance your performace as an athlete and how you can achieve drug-free pain relief.