For a personalized session and free consult, Call me: +1 334-300-0389.
Find out how ARPWave Therapy can enhance your performace as an athlete and how you can achieve drug-free pain relief.
- Understanding electrotherapy modalities
- Factors influencing electrotherapy settings
- Individual patient assessment techniques
- Adjusting parameters for optimal results
- Monitoring progress and outcomes
- Best practices for electrotherapy customization
Electrotherapy is an increasingly popular treatment modality that employs electrical currents to alleviate pain, promote healing, and enhance recovery. Understanding the different types of electrotherapy modalities is essential for making informed decisions whether you are seeking relief from chronic pain, aiming to improve athletic performance, or addressing stress-related conditions.
There are several common types of electrotherapy modalities available:
- TENS (Transcutaneous Electrical Nerve Stimulation): TENS uses low-voltage electrical currents to relieve pain by stimulating sensory nerves. It is particularly effective for conditions such as arthritis, back pain, and other musculoskeletal disorders. To maximize its benefits, consumers should use it according to their comfort level—starting with lower settings and gradually increasing as needed.
- EMS (Electrical Muscle Stimulation): EMS is designed to stimulate muscle contractions and can be beneficial for athletes looking to prevent atrophy or enhance muscle output. Utilizing EMS for specific muscle groups post-exercise can expedite recovery. It’s advisable for users to consult a professional to determine the appropriate settings and duration of use.
- IFC (Interferential Current Therapy): This method combines two medium frequency currents to create an interference pattern that can penetrate deeper into the tissues. It is effective in treating acute and chronic pain, as well as edema reduction. Users should consider placement of electrodes carefully for optimal delivery.
- Microcurrent therapy: This low-level current aids in cellular repair and is often used in aesthetic treatments for skin rejuvenation. Those interested in beauty and wellness should focus on treatment areas and discuss desired outcomes with their therapist.
When customizing your electrotherapy settings, it’s crucial to keep in mind your personal health conditions and specific goals. Begin by thoroughly researching each modality to understand its intended effects, and don’t hesitate to ask for demonstrations or guidance from a licensed professional. Effective customization often involves adjusting parameters such as frequency, intensity, and duration to suit individual tolerances and treatment objectives.
Additionally, many devices come with user-friendly settings that allow consumers to tailor their experience. For instance, a TENS device may offer different modes for pulsation and intensity, which you can experiment with to see which settings yield the best relief. Always monitor your body’s response during each session, as this feedback will help determine the most effective approach moving forward.
Incorporating electrotherapy into your wellness regimen can enhance your overall treatment experience, but understanding the nuances of each modality allows for more informed and effective use. Whether for sport recovery, pain management, or relaxation, aligning your therapy with your unique needs will help ensure successful outcomes.
Factors influencing electrotherapy settings
Electrotherapy settings are influenced by a multitude of factors that intertwine with the individual preferences and physiological responses of patients. Addressing these factors is critical to ensure that the treatment is not only effective but also safe. Key considerations include patient demographics, the nature of the condition being treated, specific treatment goals, and individual responses to electrotherapy.
One of the primary factors is the patient’s age and overall health status. Pediatric patients may require different settings compared to adults, as their tissues and systems are still developing. Similarly, older adults may have more sensitivity and comorbidities that necessitate adjustments in intensity and duration. Factors such as skin type, level of pain tolerance, and prior experiences with pain management methods will also inform the customization of electrotherapy settings.
The type of condition being treated cannot be overlooked. Acute injuries, such as sprains, often benefit from higher frequencies and lower intensities to promote muscle relaxation and pain relief. In contrast, chronic conditions might require prolonged exposure to lower frequencies to stimulate healing and improve blood circulation. Each condition may have its ideal range for frequency, intensity, and duration, which should be tailored accordingly.
A framework for understanding how patient characteristics influence treatment parameters can be summarized in the following table:
| Factor | Considerations for Settings |
|---|---|
| Age | Adjust frequency and intensity based on developmental stages and overall health. |
| Health Status | Consider comorbid conditions that may affect sensitivity to electrical stimulation; adjust settings accordingly. |
| Type of Condition | Alter parameters to either stimulate or relax the specific tissues, depending on whether the condition is acute or chronic. |
| Patient Tolerance | Start with conservative settings for new users, then gradually increase based on feedback and comfort level. |
| Previous Experiences | Assess prior treatment responses to inform adjustments to ensure successful outcomes. |
In addition, monitoring patient feedback during and after treatments becomes essential for continuous adjustments. This ongoing dialogue helps clinicians fine-tune electrotherapy settings based on real-time responses. For example, if a patient reports discomfort, it may be necessary to reduce the intensity or modify electrode placements. Conversely, if a patient feels minimal effect, increasing the intensity or changing frequency may yield better outcomes.
Another influential element is the provider’s expertise and familiarity with various electrotherapy modalities. Different practitioners may have preferences for certain settings based on anecdotal evidence or clinical experiences that can further enhance treatment customization. Collaborating with a registered therapist can lead to optimized settings, tailored exercises, and synergistic modalities, creating a comprehensive treatment plan effectively addressing the patient’s needs.
Ultimately, personalization of electrotherapy settings is not a static endeavor but a dynamic process that relies on an amalgamation of the factors discussed. Customizing these settings results in a tailored approach to therapy that significantly enhances the likelihood of achieving successful outcomes in pain relief, recovery, and overall well-being.
Individual patient assessment techniques

Individual patient assessment techniques are essential in customizing electrotherapy settings to achieve successful outcomes. A thorough assessment allows practitioners to gather pertinent information about each patient’s unique situation, physical condition, and therapeutic goals. This tailored approach not only enhances the effectiveness of treatment but also minimizes any risks involved in the electrotherapy process.
To begin with, practitioners should conduct a detailed medical history review. This includes understanding the patient’s past and present health issues, any previous surgeries, medications, and other treatments they have undergone. This groundwork is critical for identifying potential contraindications to specific electrotherapy modalities and settings. For example, individuals with certain implanted devices, such as pacemakers, should avoid electrical stimulation around the device area.
Next, conducting a physical examination is vital to assess the affected areas directly. This may involve evaluating muscle strength, joint range of motion, and the extent of pain or discomfort. Using standardized assessment tools, such as the Visual Analog Scale (VAS) or the Oswestry Disability Index, can help quantify pain levels and functionality, providing a solid benchmark for measuring progress.
Subjective reporting from the patient is equally important. Patients should be encouraged to describe their symptoms, including pain characteristics—such as intensity, duration, and factors that exacerbate or alleviate their condition. This self-reporting helps tailor the approach further by allowing adjustments to frequency, intensity, and treatment duration based on the patient’s feedback.
In addition to symptoms, assessing lifestyle factors is paramount. Understanding a patient’s daily activity levels, occupational stresses, and recreational pursuits can aid in customizing settings more effectively. For example, an athlete may require different electrotherapy settings for muscle recovery compared to a corporate executive seeking stress relief. Identifying specific goals, whether it’s improving athletic performance or managing chronic pain, will help direct the type of electrotherapy and its parameters.
Functional assessments also play a crucial role in the evaluation process. These tests gauge how effectively a patient can perform specific activities related to their daily life or sport. By analyzing the results, practitioners can align electrotherapy settings with the patient’s functional requirements, ensuring that treatment enhances not only pain relief but also overall functionality and quality of life.
Another aspect of patient assessment involves monitoring psychological factors. Emotional health significantly influences physical conditions and responses to treatment. Anxiety and stress can exacerbate pain, so understanding a patient’s psychological state may guide practitioners in choosing where to focus their electrotherapy efforts. Techniques such as relaxation training or mindfulness may complement electrotherapy treatments effectively.
Finally, follow-up assessments after initiating electrotherapy treatment are crucial. Regularly scheduled sessions will provide opportunities for reassessing the patient’s response and make necessary adjustments to the electrotherapy settings. This ongoing feedback loop allows for modifications based on observed changes in pain levels, functional abilities, and overall treatment outcomes, reinforcing the importance of adaptability in therapy.
A comprehensive approach to individual patient assessment incorporates medical history, physical evaluations, lifestyle factors, functional tests, psychological insights, and continuous monitoring. By adopting these techniques, practitioners can ensure that electrotherapy settings are finely customized, leading to more effective and successful therapeutic outcomes for a diverse range of patients that includes athletes, corporate executives, and those seeking pain relief or stress alleviation.
Adjusting parameters for optimal results
 Adjusting the parameters of electrotherapy, such as frequency, intensity, and duration, is pivotal in achieving optimal results tailored to the patient’s needs. Each of these factors plays a crucial role in how the body responds to treatment. Frequency, for instance, refers to the number of electrical pulses delivered per second, impacting the physiological responses required for therapeutic effects. A higher frequency typically stimulates sensory nerves, while lower frequencies target deeper tissue and promote muscle contractions. Selecting the right frequency based on the patient’s condition is essential for maximizing relief and enhancing recovery.
Adjusting the parameters of electrotherapy, such as frequency, intensity, and duration, is pivotal in achieving optimal results tailored to the patient’s needs. Each of these factors plays a crucial role in how the body responds to treatment. Frequency, for instance, refers to the number of electrical pulses delivered per second, impacting the physiological responses required for therapeutic effects. A higher frequency typically stimulates sensory nerves, while lower frequencies target deeper tissue and promote muscle contractions. Selecting the right frequency based on the patient’s condition is essential for maximizing relief and enhancing recovery.
Intensity refers to the strength of the electrical current, and it is vital to adjust this based on the patient’s comfort and tolerance levels. Starting with lower intensity is advisable, particularly for newcomers to electrotherapy, to avoid discomfort or adverse reactions. Gradually increasing intensity allows patients to adapt and can lead to more effective pain relief. Monitoring the patient’s feedback during sessions can guide clinicians in making real-time adjustments to ensure that the intensity remains effective without causing distress.
Duration encompasses the length of each treatment session. The optimal duration may vary depending on the treatment goals and individual responses. Acute pain conditions may benefit from shorter, more frequent sessions, while chronic conditions often respond well to longer durations to facilitate muscle relaxation or tissue healing. It’s important to find a balanced approach that maximizes comfort while achieving therapeutic objectives.
Incorporating feedback and observations from each session empowers practitioners to finely tune electrotherapy settings. For instance, if a patient indicates that a particular setting felt particularly effective, clinicians can prioritize similar settings in subsequent treatments. Conversely, if a patient reports discomfort, it may necessitate a prompt reassessment of the settings involved.
Therapists may utilize a combination of treatments to further improve outcomes. For example, blending TENS and EMS within a single session can provide both pain management and muscle strengthening, catering to a multi-faceted therapeutic approach. Likewise, strategic electrode placement should not be overlooked; proper placement can significantly enhance the efficacy of the treatment by optimizing electrical flow to the target area.
Understanding the interactions between various settings can aid in customizing the electrotherapy experience. For instance, utilizing a higher pulse width in conjunction with a moderate frequency may enhance comfort while ensuring effective stimulation of target muscles or nerves. Collaborating with patients to develop a personalized treatment plan that incorporates their unique feedback and response patterns is essential for long-term success.
“The effectiveness of electrotherapy is not just determined by the technology itself but also by how well it is tailored to fit the individual patient’s needs.” – Expert in Electrotherapy
With a systematic approach to adjusting the above parameters and engaging patients in their treatment plans, practitioners can enhance the likelihood of achieving successful outcomes through electrotherapy. Each consideration feeds into a broader strategy of customization that ultimately leads to more effective and satisfying experiences for patients.
Monitoring progress and outcomes
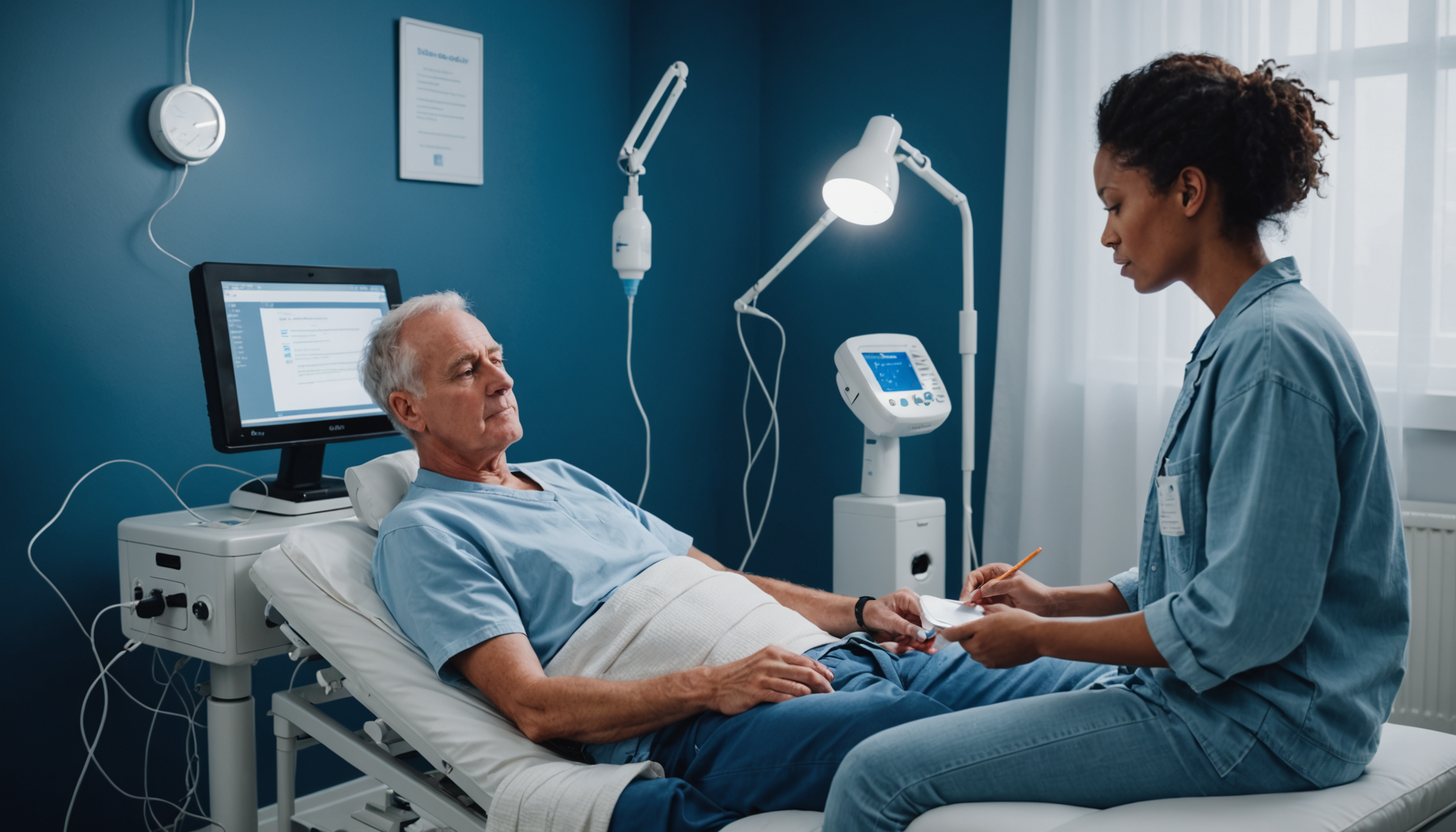 Monitoring the effects of electrotherapy is a continuous process that is paramount in tailoring treatments for maximum effectiveness. One of the critical aspects of monitoring is to regularly assess the patient’s responses throughout the treatment, taking into account both physical and subjective feedback. This feedback loop not only aids in refining the settings but also deepens the clinician-patient relationship, fostering an environment of trust and collaboration.
Monitoring the effects of electrotherapy is a continuous process that is paramount in tailoring treatments for maximum effectiveness. One of the critical aspects of monitoring is to regularly assess the patient’s responses throughout the treatment, taking into account both physical and subjective feedback. This feedback loop not only aids in refining the settings but also deepens the clinician-patient relationship, fostering an environment of trust and collaboration.
Patients are encouraged to articulate their experiences during and after each session—did the treatment alleviate their pain, enhance function, or induce discomfort? Keeping a treatment diary can be beneficial, allowing patients to record their feelings and any changes in symptoms over time. The data gathered can be invaluable for clinicians, enabling them to pinpoint what strategies are working and where adjustments may be necessary. Comprehensive documentation of these progress reports helps establish a baseline for treatment efficacy and guides further modifications.
Physical assessments should also play a crucial role in monitoring progress. Clinicians can track changes in muscle strength, range of motion, and pain levels using validated tools and scales. Regular evaluations can indicate whether the selected electrotherapy settings remain appropriate and beneficial or if they need fine-tuning. Should a patient’s condition evolve, the strategy must evolve as well, adjusting intensity, frequency, and duration accordingly to maintain successful outcomes.
In addition, monitoring should encompass the evaluation of functional improvements, helping to assess how well the therapy is translating into daily life activities or athletic performance. As patients begin to experience enhanced mobility or reduced pain, setting new goals can help keep the motivation high and lead to continued progress. For instance, if an athlete sees improvements in recovery times, the focus may shift towards enhancing performance further through advanced modality customization.
Moreover, patient education on self-monitoring techniques can significantly enhance the effectiveness of the electrotherapy experience. Teaching patients how to assess their own response to treatment—such as recognizing signs of over-stimulation or observing patterns of pain relief—will empower them, enabling a more proactive role in their healing journey. When patients engage in their own monitoring, they can report more accurately on what aspects of the therapy are beneficial or otherwise, allowing for a more responsive treatment plan.
Adopting an adaptive, dynamic approach to monitoring not only fosters transparency but also cultivates a culture of personalized care that embraces the unique journey of each patient. Assessing progress in real time and making ongoing adjustments creates a cycle of improvement, enhancing the likelihood of achieving the successful outcomes desired. A rigorous monitoring framework leads to insights that make customizing electrotherapy settings worthwhile, turning data collected into actionable strategies that are fine-tuned for individual needs.
- What is electrotherapy?
- Electrotherapy is a treatment that uses electrical currents to promote healing, relieve pain, and improve muscle function. It’s commonly utilized in physical therapy to aid in recovery from injuries and chronic pain conditions.
- How do I know which electrotherapy modality is best for me?
- Your choice of electrotherapy modality should depend on your specific condition, treatment goals, and personal preferences. Consulting with a licensed professional can help identify the most suitable approach for your needs.
- Are there any risks associated with electrotherapy?
- While generally safe, electrotherapy may pose risks for individuals with certain medical conditions such as pacemakers or seizures. It’s essential to discuss your medical history with a healthcare provider before beginning treatment.
- How often should I be receiving electrotherapy treatments?
- The frequency of electrotherapy sessions can vary based on the individual’s condition and treatment plan. Some may require daily sessions, while others might benefit from once a week or less, as determined by a professional.
- Can I use electrotherapy at home?
- Many electrotherapy devices are available for home use, but it’s critical to use them under the guidance of a healthcare provider to ensure safety and effectiveness. Start with professional advice on settings and techniques.
- How quickly can I expect to see results from electrotherapy?
- Results can vary depending on the individual and the condition being treated. Some may experience immediate relief, while others may require several sessions before noticing significant improvements.
- What should I do if I experience discomfort during electrotherapy?
- If you experience discomfort, it’s essential to communicate this to your practitioner immediately. Adjustments to the settings or techniques may be necessary to enhance comfort and effectiveness.
Best practices for electrotherapy customization

When incorporating electrotherapy into any treatment plan, adhering to best practices for customization can significantly enhance the therapy’s effectiveness and ensure successful outcomes. Firstly, practitioners should prioritize clear communication with patients to understand their distinct needs and preferences. This dialogue helps to establish mutual expectations regarding pain management, recovery timelines, and comfort levels.
One effective approach to customization is to employ a comprehensive baseline assessment before initiating treatment. This may include gathering information on the patient’s medical history, current health status, lifestyle, and specific therapeutic goals. For example, an athlete may have different recovery priorities compared to someone managing chronic pain. This distinction allows practitioners to tailor electrotherapy settings such as frequency and intensity accordingly.
Another critical practice is to implement a trial-and-error methodology. Patients respond differently to various electrotherapy modalities. By starting with conservative settings—low intensity and moderate frequency—and gradually adjusting based on patient feedback, practitioners can determine the most effective electrotherapy settings for individual cases. Patients should be encouraged to report their experiences actively, noting what feels effective or uncomfortable during each session.
Regular follow-up assessments are essential for evaluating the progress and effectiveness of the therapy. These reevaluations allow clinicians to adjust the settings or approaches as needed. For instance, if a patient reports increased strength or decreased pain over time, it may be beneficial to revisit the therapy parameters to optimize results further. Conversely, should discomfort or minimal progress arise, it may prompt a reassessment of electrode placements and treatment settings.
Electrode placement also plays a pivotal role in customizing electrotherapy treatments. Proper positioning can enhance the effectiveness of each modality. For example, in TENS therapy, placing electrodes around the painful area rather than directly over it may yield better pain relief. Practitioners should educate patients on this aspect, empowering them to adjust their home-use devices effectively.
Moreover, documenting patient responses throughout the treatment process is crucial. Keeping a treatment log can help track changes and patterns over time, facilitating informed decision-making for future sessions. Patients can jot down notes regarding pain levels, mood changes, and overall treatment satisfaction which can provide invaluable insights during follow-ups.
Lastly, integrating patient preferences into the treatment plan is essential for improving adherence and satisfaction. Offering patients choices regarding dosage levels, duration of treatments, and types of modalities can lead to a more personalized experience. For instance, some may prefer short, intense sessions for quick relief, while others might benefit from extended sessions aimed at relaxation and stress reduction.
Customizing electrotherapy treatments is a dynamic process that thrives on patient involvement, continuous assessment, and adaptive strategies. By following these best practices, practitioners can significantly enhance the likelihood of achieving successful outcomes, leading to improved quality of life for their patients.
For a personalized session and free consult, Call me: +1 334-300-0389.
Find out how ARPWave Therapy can enhance your performace as an athlete and how you can achieve drug-free pain relief.