For a personalized session and free consult, Call me: +1 334-300-0389.
Find out how ARPWave Therapy can enhance your performace as an athlete and how you can achieve drug-free pain relief.
- Techniques for effective electrotherapy training
- Understanding electrotherapy modalities
- Assessing patient readiness for electrotherapy
- Demonstrating equipment usage
- Monitoring patient progress and feedback
- Ensuring adherence to treatment protocols
When training patients in using electrotherapy, it is crucial to employ a variety of effective techniques that cater to their individual needs and circumstances. This involves understanding the patient’s pain management goals, their previous experiences with pain relief therapies, and their comfort level with technology.
Start by establishing a trusting relationship with your patients. Taking time to listen to their concerns and preferences will enable you to tailor your training approaches accordingly. This initial engagement will help create a supportive environment conducive to learning and confidence.
Demonstration plays a vital role in effective training. Patients benefit from seeing how electrotherapy equipment is set up and operated. A walk-through of the device’s features and functionalities, including buttons, settings, and safety precautions, allows patients to familiarize themselves with the technology before usage. Consider using video demonstrations or printed instructions as supplementary materials, reinforcing the training session.
It is also essential to simplify instructions. Use plain language and avoid medical jargon that may confuse patients. For instance, when describing adjustments for comfort levels during electrotherapy sessions, use relatable analogies, such as comparing sensations to feeling “warm” or “tingly” rather than technical terms. This will help patients feel more at ease and willing to experiment with the settings on their own.
Role-playing can be an effective technique as well. Encourage patients to practice setting up and using the equipment under your supervision. This hands-on experience can significantly enhance their confidence. Monitor their technique closely, providing constructive feedback and encouragement throughout the process.
Additionally, leverage technology to facilitate ongoing learning and adherence. Consider creating a dedicated online platform or forum where patients can ask questions, share experiences, and receive tips about using electrotherapy. This community approach fosters a sense of belonging and accountability, which can be very motivating.
Lastly, emphasize the importance of consistency in using electrotherapy for optimal results. Educate patients about incorporating this therapy into their regular routines, suggesting they set reminders for sessions or keep a journal to track their progress and any changes in their symptoms. By guiding them in setting achievable goals, you empower patients to take charge of their treatment journey.
Understanding electrotherapy modalities
Electrotherapy encompasses a range of modalities, each designed to address specific conditions and patient needs. Understanding these different modalities is fundamental for both practitioners and patients to ensure effective treatment and optimal results.
The primary electrotherapy modalities include TENS (Transcutaneous Electrical Nerve Stimulation), NMES (Neuromuscular Electrical Stimulation), and interferential current therapy. Each modality has distinct mechanisms of action and therapeutic applications.
| Modality | Mechanism | Applications | Considerations |
|---|---|---|---|
| TENS | Stimulates sensory nerves to inhibit pain signals | Pain management, post-surgery relief, chronic pain conditions | Adjust settings based on patient comfort; duration of treatment may vary |
| NMES | Stimulates motor nerves to enhance muscle contraction | Muscle rehabilitation, preventing muscle atrophy, improving blood circulation | Monitor muscle response; inappropriate settings can lead to discomfort or injury |
| Interferential Current Therapy | Uses two medium frequency currents to produce a deeper stimulation | Reducing pain and inflammation, enhancing circulation | Requires precise placement of electrodes; patient feedback is crucial for effectiveness |
It is essential for patients to recognize the specific indications for each type of electrotherapy and how they relate to their personal treatment goals. For instance, patients aiming primarily for pain relief may benefit more from TENS, while those focusing on muscle recovery might find NMES more suitable. Introducing these modalities during the training sessions allows patients to engage with the technology more confidently, as they can see how it aligns with their treatment objectives.
Additionally, while patients learn about different modalities, they should be educated on the specific settings and parameters associated with each therapy. For example, understanding how frequency and pulse duration affect the sensation and effectiveness of TENS can empower patients to adjust their treatment to maximize comfort while enhancing outcomes.
Patient feedback is crucial in this context. Encouraging patients to share their experiences when trying different techniques fosters a collaborative approach to their therapy. This feedback loop can help refine the use of electrotherapy modalities and keep the practitioner informed about what works best for each individual, ultimately leading to improved adherence to treatment protocols and better overall results.
In summary, a solid understanding of the various electrotherapy modalities—accompanied by sensitive guidance and patient education—enables both patients and practitioners to work together toward effective pain management and rehabilitation strategies.
Assessing patient readiness for electrotherapy
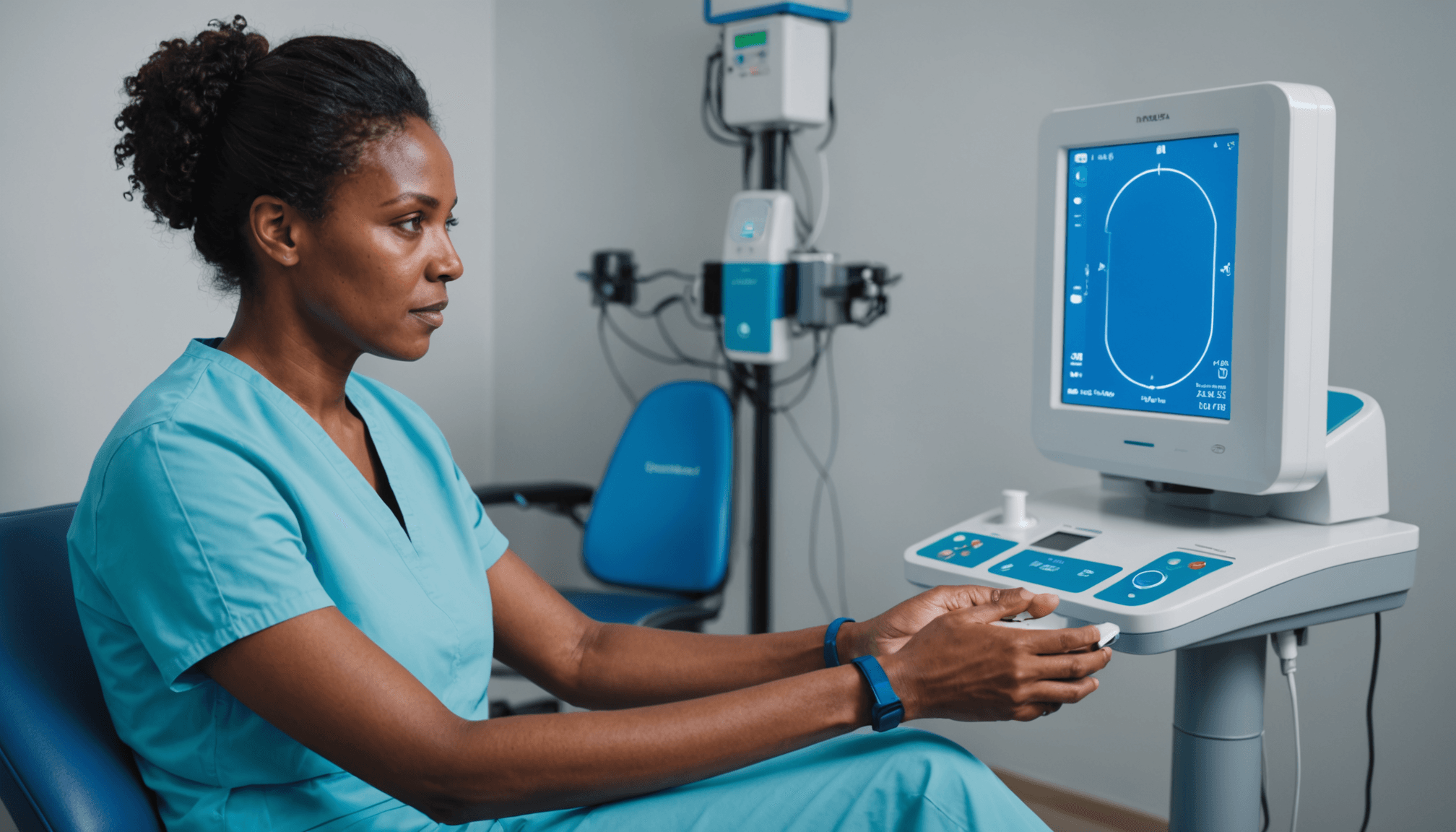
Assessing patient readiness for electrotherapy involves a comprehensive evaluation that considers physical, emotional, and cognitive factors. It’s vital to ensure that patients fully understand the therapy, feel confident in their ability to use the equipment, and are mentally prepared for the treatment process.
Start by conducting a thorough initial assessment that includes questioning the patient about their medical history, current symptoms, and any previous experiences with electrotherapy or other pain management techniques. Creating an open dialogue allows patients to express their concerns and expectations regarding therapy, and helps you gauge their understanding of the process.
Here are some key factors to assess:
- Physical Readiness: Ensure that the patient’s physical condition allows for electrotherapy. Certain conditions, such as pacemakers or skin irritations at the site of electrode placement, may contraindicate the use of electrotherapy. Discussing these factors openly can help prevent complications.
- Cognitive Understanding: Evaluate the patient’s comprehension of how electrotherapy works and its intended outcomes. This includes explaining the sensation they may feel during treatment and addressing any misconceptions they might have.
- Emotional and Psychological Readiness: Consider the patient’s psychological state. A patient who is anxious or fearful might need additional support, such as reassurance or education about the technology, to help them feel more comfortable.
Utilizing visual and hands-on demonstrations can significantly enhance understanding. Encourage patients to observe and interact with the equipment before their first treatment. This can alleviate fear and uncertainty while also providing an opportunity to review any questions they may have.
Active involvement in the training process can also promote readiness. Allow patients to articulate their expectations and any concerns regarding their treatment regimen. By creating an environment where patients feel safe to express doubts, you foster greater adherence and motivation. Consider using open-ended questions to facilitate discussion, such as:
- What are your primary goals for using electrotherapy?
- How do you feel about trying this new approach to manage your pain?
- Are there any specific concerns you have about the therapy or the equipment?
Furthermore, establish a clear set of instructions for patients on how to prepare for their electrotherapy sessions. Advise them on what to wear, how to care for their skin, and any pre-treatment measures they may need to undertake. Emphasizing the importance of these steps reinforces the patient’s sense of ownership over their treatment plan.
Engaging the patient in setting realistic expectations also plays a critical role. Help them understand that while some may experience rapid relief from symptoms, others might require several sessions to see significant changes. Maintaining open lines of communication about progress and any issues that arise encourages patients to stay invested in their treatment journey.
Finally, be observant of non-verbal cues during your interactions with the patient. Signs of discomfort or hesitation can indicate a lack of readiness. If you identify these issues, take the time to address them before proceeding with the treatment.
By thoroughly assessing a patient’s readiness for electrotherapy, you lay the groundwork for a successful treatment strategy that empowers them to take an active role in their healing process.
Demonstrating equipment usage
 Demonstrating equipment usage is a pivotal aspect of training patients in using electrotherapy effectively. A clear, step-by-step demonstration ensures that patients not only understand how to operate the equipment but also feel confident in their ability to use it independently. Begin with familiarization, showing patients the equipment upfront, pointing out crucial components like the power switch, settings dials, and electrode pads.
Demonstrating equipment usage is a pivotal aspect of training patients in using electrotherapy effectively. A clear, step-by-step demonstration ensures that patients not only understand how to operate the equipment but also feel confident in their ability to use it independently. Begin with familiarization, showing patients the equipment upfront, pointing out crucial components like the power switch, settings dials, and electrode pads.
During the demonstration, use deliberate movements and clear explanations to guide patients through the setup process. For instance, when attaching electrodes, explain their placement in relation to the treatment area and discuss the importance of clean, dry skin for optimal adhesion. This attention to detail in demonstration helps patients grasp the significance of proper setup, thereby increasing the likelihood of effective treatment outcomes.
“Teaching is not just telling; it is showing, guiding, and providing opportunities for practice.”
Incorporating interactive elements during the demonstration can heighten engagement. Encourage patients to ask questions as you walk through the process. This not only clarifies their doubts but also reinforces their learning. After demonstrating how to operate the equipment, allow the patient to try it under your supervision. This practical experience is invaluable, as it transforms theoretical understanding into practical application.
When patients begin using the equipment, emphasize the importance of following specific protocols, such as adjusting intensity levels and duration based on their comfort. Guide them through the initial settings and encourage them to pay attention to their bodily responses. Remind them that discomfort should be reported immediately, establishing a baseline for communication about sensations experienced during treatment.
Using analogies can be an effective strategy for explaining technical aspects of the equipment. For instance, comparing the sensation of electrotherapy to familiar experiences, like a gentle massage or the mild prick of a static shock, can help demystify the process. By contextualizing their experiences with relatable terms, patients are more likely to understand what to expect during their sessions.
Moreover, reiterate the significance of safety precautions, such as ensuring that the device is turned off when not in use and maintaining the integrity of the electrodes. Reinforcing these practices fosters a sense of responsibility in patients, which is crucial for their overall adherence to the treatment protocol.
After the demonstration and initial usage, solicit feedback from patients about their comfort and understanding of the process. This dialogue is essential for tailoring ongoing training and support. Encourage patients to share their feelings about the experience and any concerns that arise as they become more accustomed to using the device. This feedback loop not only enhances the training process but also serves as a foundation for building patient confidence and ensuring they can effectively manage their therapy independently.
In summary, demonstrating equipment usage with clarity and engagement, while fostering an environment of communication and support, empowers patients. This approach ensures they are fully equipped to use electrotherapy techniques confidently and safely as part of their pain management journey.
Monitoring patient progress and feedback
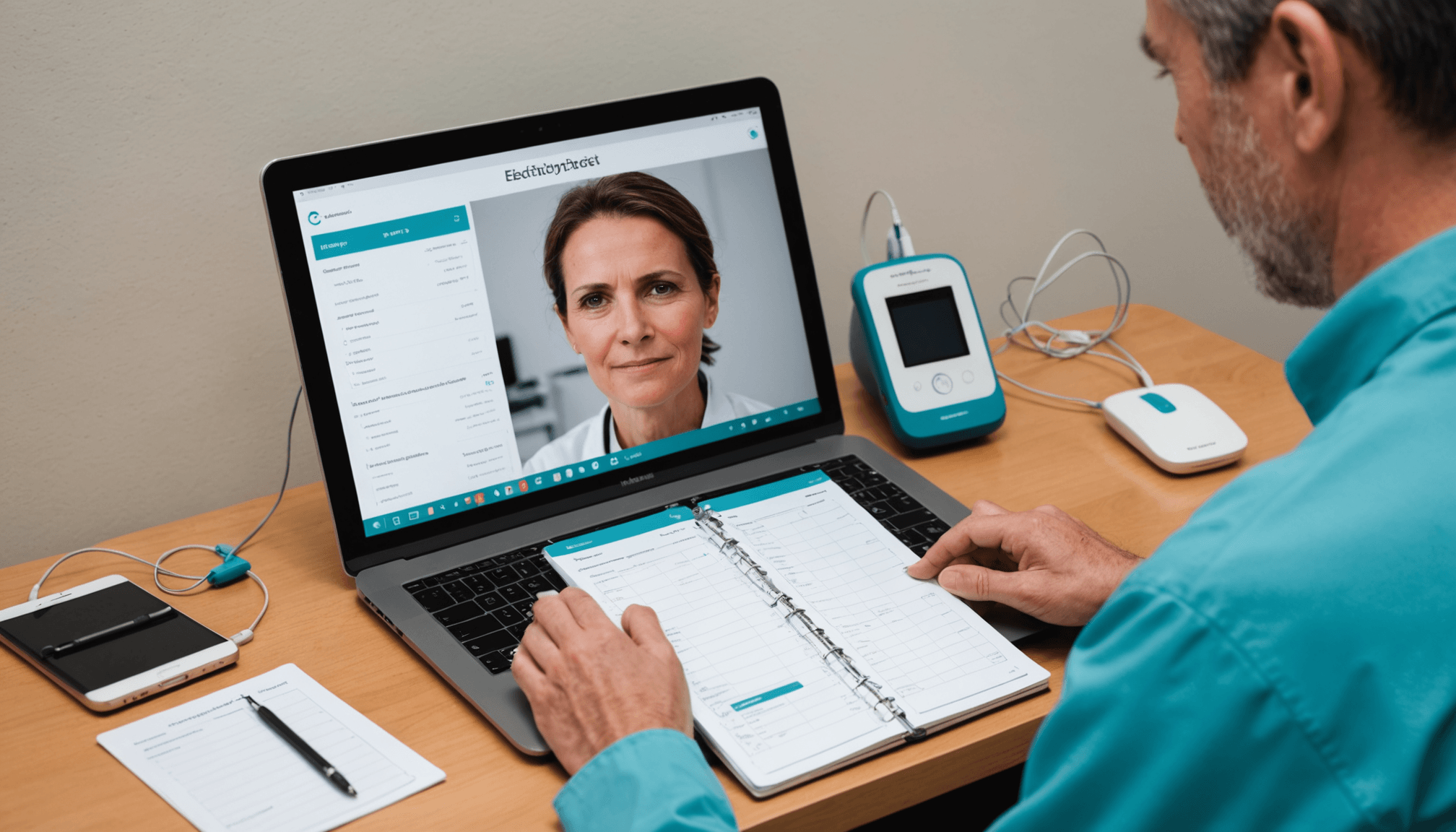 Monitoring patient progress involves systematically recording and evaluating data related to the patient’s treatment experience and outcomes. This process plays a crucial role in ensuring that electrotherapy is effectively addressing the individual’s needs. Establishing clear benchmarks for success during training helps to keep both the practitioner and the patient focused on the treatment goals. Regular check-ins and assessments of progress not only aid in recognizing improvements but also offer opportunities for timely adjustments to the treatment plan.
Monitoring patient progress involves systematically recording and evaluating data related to the patient’s treatment experience and outcomes. This process plays a crucial role in ensuring that electrotherapy is effectively addressing the individual’s needs. Establishing clear benchmarks for success during training helps to keep both the practitioner and the patient focused on the treatment goals. Regular check-ins and assessments of progress not only aid in recognizing improvements but also offer opportunities for timely adjustments to the treatment plan.
Incorporating a systematic approach to tracking progress is essential. Create and maintain a treatment log where patients can document session dates, durations, settings used, and subjective changes in pain levels or mobility after treatment. This record gives patients a tangible way to visualize their journey, much like an athlete tracking performance metrics. From these logs, you can identify patterns and make evidence-based decisions regarding future treatments.
Encouraging feedback immediately following sessions is equally important. Patients’ perceptions of their experiences can reveal invaluable insights into their comfort levels and the effectiveness of the treatment. Ask open-ended questions like, “How did you feel during and after the session?” or “Was there anything you found challenging or surprising?” This dialogue allows patients to take ownership of their care and reinforces the practitioner-patient partnership.
It is crucial to be responsive to patient feedback. If a patient reports discomfort or ineffective outcomes, consider revisiting treatment modalities, electrode placements, or even setting adjustments. Recognizing the influence of individual patient responses is pivotal to tailoring therapy to specific needs. Training should be adaptable, addressing any evolving barriers that patients may face, fostering resilience through continuous support.
Additionally, closely monitor patients’ emotional responses as they undergo treatment. Electrotherapy can provoke anxiety or uncertainty in some individuals, particularly in the early stages. Conducting supportive discussions regarding their concerns, whether they are related to equipment usage or the therapy’s effectiveness, creates a safe space for patients. This trust and transparency can significantly enhance their commitment to the treatment process.
Adherence to treatment protocols is another critical area of focus during the monitoring process. Consistency in using the therapy, coupled with adherence to the established schedule, will ultimately lead to the best outcomes. Encourage patients to establish a routine, possibly by combining electrotherapy sessions with daily activities or utilizing reminders. This strategy can help integrate electrotherapy into their lives more seamlessly, fostering a commitment that often translates into better outcomes.
Moreover, utilizing technology to streamline feedback and monitoring can optimize the process. Consider employing wearable devices or mobile apps that allow for real-time tracking and communication of symptoms and treatment effects. These tools not only facilitate patient engagement but also provide a wealth of data that can be shared and analyzed to further refine treatment approaches.
By embedding comprehensive monitoring practices into electrotherapy training, both patients and practitioners can cultivate a responsive therapeutic environment. This dynamic interaction encourages continuous learning, adjustments in care, and ultimately a more successful treatment journey that is well-informed and patient-centered.
- What types of progress should I track during electrotherapy treatment?
- Track symptoms such as pain levels, mobility improvements, and any side effects experienced during or after sessions. Keeping a treatment log that includes these details can provide valuable insights into the effectiveness of electrotherapy.
- How often should I communicate with my practitioner about my progress?
- Regular communication is key. Aim to provide feedback after each session, but also seek out discussions during scheduled appointments to discuss ongoing experiences and any concerns that may arise.
- What should I do if I feel discomfort during a session?
- If you experience discomfort, it’s crucial to inform your practitioner immediately. They can help adjust the settings or electrode placement to ensure your treatment is both safe and effective.
- Can I use electrotherapy alongside other pain management treatments?
- Yes, electrotherapy can often complement other treatments like physical therapy or medications. However, always discuss any combination therapies with your healthcare provider to ensure safety and efficacy.
- What are some common side effects of electrotherapy?
- Common side effects may include mild skin irritation at the electrode sites or temporary muscle soreness. Discuss any prolonged or severe reactions with your practitioner for guidance.
- How can I remain motivated to continue my treatment?
- Setting realistic goals and tracking your progress can help maintain motivation. Celebrate small victories and stay in touch with your practitioner to receive encouragement and support throughout your journey.
- Is it normal to not see immediate results from electrotherapy?
- Yes, it’s common for patients not to experience immediate relief. Electrotherapy can take time to show its effectiveness, and consistent usage according to your treatment plan is vital for optimal results.
Ensuring adherence to treatment protocols

Ensuring adherence to treatment protocols is essential for the success of electrotherapy as a pain management technique. Patients benefit significantly when they actively engage in their treatment plans, which reinforces their commitment to the prescribed therapy. This engagement begins with providing clear and comprehensive instructions regarding the electrotherapy regimen.
First, it’s crucial to set realistic and achievable goals with patients. Help them understand what the treatment entails and how it integrates into their overall pain management strategy. Utilize SMART goals—specific, measurable, achievable, relevant, and time-bound objectives—to outline what patients can expect over a defined period. For example, a goal could be to reduce pain levels by a certain percentage within a month of consistent electrotherapy use.
To facilitate adherence, encourage patients to develop a routine that incorporates their electrotherapy sessions seamlessly into their daily lives. Suggestions may include setting specific times for treatment or linking it to other daily activities, such as watching a show or listening to music. Utilizing mobile apps that send reminders about upcoming sessions can also enhance consistency.
Another vital aspect of adherence is education regarding the importance of consistency. Patients must understand that missing sessions can lead to setbacks in their progress. Educate them on how electrotherapy works, emphasizing that regular use generally yields better outcomes and faster relief from symptoms. Discuss the significance of attending all scheduled appointments and consistently following the recommended home regimen.
Incorporating a feedback loop is also essential for adherence. Encourage ongoing communication about their experiences with electrotherapy. Questions such as “How do you feel after your treatment?” or “Have you noticed any changes since starting your sessions?” can prompt meaningful dialogue. This engagement not only empowers patients but also provides insights that can be used to adjust treatment plans if necessary.
Moreover, foster a supportive environment that recognizes and rewards adherence. Celebrate patients’ milestones, whether they reach a pain threshold goal or successfully integrate electrotherapy into their routine. This positive reinforcement can serve as motivation, prompting them to remain dedicated to their treatment plans.
Finally, periodic re-evaluations of treatment protocols are fundamental. As patients progress, their needs and symptoms may change. Schedule regular check-ins to assess their pain levels, treatment efficacy, and any new concerns that might arise. This ongoing assessment not only helps keep the treatment tailored to the patient’s needs but also cultivates a sense of partnership between the practitioner and the patient, reinforcing adherence to their therapy schedule.
By implementing these strategies, practitioners can significantly enhance patient adherence to electrotherapy treatment protocols, which ultimately leads to more successful outcomes in pain management.
For a personalized session and free consult, Call me: +1 334-300-0389.
Find out how ARPWave Therapy can enhance your performace as an athlete and how you can achieve drug-free pain relief.